Dozens of deaths of middle-aged Britons have been linked to blockbuster weight loss jabs, the Daily Mail can reveal.
Amid the booming popularity of Ozempic, Mounjaro and Wegovy, drug watchdogs have received 52 fatal reports for GLP-1 injections since the beginning of 2024.
Experts today sounded an alarm over the death toll, with millions more in line to get the jabs to curb the nation’s bulging waistline.
Tam Fry, chair of the National Obesity Forum, claimed that, although the drugs were hugely effective for those who need them, they were being used ‘inappropriately’ by slimmer adults who ‘fancy losing a bit of weight’.
He added: ‘If you take them and you don’t need them, and you break the rules, you run the risk of serious complications – or death.
‘People think “its not going to happen to me” but it will happen to them. So they take them and they get severe complications.’
The data, kept by a Government body, does not state whether any of the people who died while using the jabs had been using them inappropriately.
In total, the Medicines and Healthcare products Regulatory Agency (MHRA), which polices the safety of every drug used in Britain, has received 173 ‘reports with fatal outcomes’ from GLP-1 injections.
Reports of side effects have risen in line with soaring prescriptions, with the drugs’ jaw-dropping weight loss effects helping in the war on obesity.
Estimates suggest that 1.5million people in the UK are taking weight loss jabs through private online pharmacies, while 200,000 are doing so through the NHS.
Yet concerns are growing over the side effects, with milder ones including headaches, vomiting and diarrhoea.
In more serious cases, GLP-1s can cause gallstones, kidney stones and inflammation of the pancreas, with some doctors warning of ‘life-threatening complications’.
Two of the reported deaths were adults in their 20s, as revealed by our investigation into the MHRA’s Yellow Card scheme.
Yet the bulk were among middle-aged adults, with eight deaths logged in people in their 30s, 15 in their 40s, and 37 in their 50s.
A death reported to the MHRA does not necessarily mean it has been caused by the medicine – only that someone had a suspicion it may have been.
The death may have been entirely coincidental, health chiefs warn.
Underlying or concurrent illnesses and other medicines the patients may have been taking at the time of their death may be responsible. Obesity, for example, is known to cause cancer and heart disease – some of the UK’s biggest killers.
But given how popular the drugs are becoming, experts warn the MHRA’s figures might be the tip of the iceberg.
It is not essential to report side effects to the MHRA and only one in ten serious reactions end up being reported to them, according to estimations.
It comes after a Scottish nurse last year became the first person in Britain whose death was directly linked to a weight-loss jab.
Susan McGowan, 58, suffered multiple organ failure, septic shock and pancreatitis after taking two low-dose injections of Mounjaro, also known as tirzepatide.
She bought the powerful drug from an online pharmacy but died at University Hospital Monklands in Airdrie on September 4, 2024.
Her death certificate listed multiple organ failure, septic shock and pancreatitis as the immediate cause of death – but ‘the use of prescribed tirzepatide’ was recorded as a contributing factor.
The MHRA’s Yellow Card data hub was set up in the wake of the thalidomide scandal in the 60s, allowing doctors, pharmacists and patients themselves to report adverse reactions thought to be caused by drugs used in Britain.

Scottish nurse Susan McGowan, 58, who experienced multiple organ failure, septic shock and pancreatitis after taking just two doses of Mounjaro
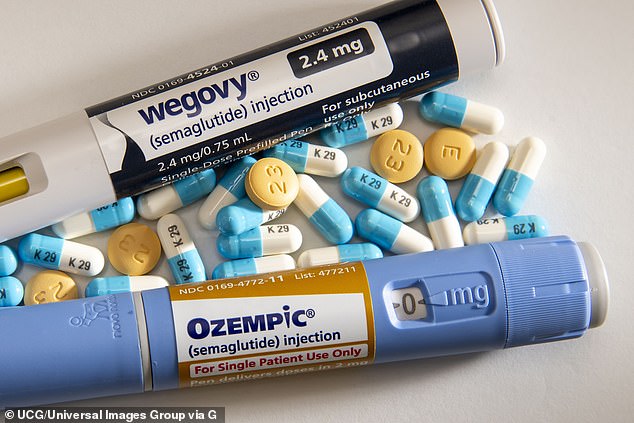
Drug watchdogs have received 52 fatal reports for fat jabs since the beginning of 2024 when they started to be rolled out en masse
This can lead to them being reviewed, having warnings placed on their labels, or being taken off the market completely.
Every drug approved for use in Britain has to go through rigorous safety trials before being made available to the public but some issues can slip under the radar, such as the rare blood clots triggered by AstraZeneca’s Covid vaccine.
Drugs newly brought to market, including Ozempic and Mounjaro, also fall under another MHRA safety scheme called the Black Triangle.
This gives the drugs this symbol (▼), identifying them as medicines that require additional monitoring.
The Mail’s analysis found exenatide, branded as Bydureon, was linked to 55 deaths – more than any of the other five GLP-1’s included in the audit.
It is only prescribed to treat type 2 diabetes, the same as two other GLP-1s included in the investigation: dulaglutide (Trulicity) and lixisenatide (Suliqua).
Thirty-one deaths were marked against semaglutide, the hunger-banishing chemical behind both Ozempic and Wegovy.
Tirzepatide, the powerful ingredient in Mounjaro, was linked to 38.
The MHRA says the numbers might be inflated as some cases could have multiple GLP-1s listed as suspected drugs, meaning they are counted twice.
Doctors insist that fat jabs will be ‘game changers’ when it comes to fighting back against Britain’s long-running problem of obesity, which costs the economy an estimated £100billion per year.
Hundreds of thousands take the drugs safely and have been doing so for years, which experts say has finally let them shed the pounds that they otherwise could not have shifted.
Doctors insist that fat jabs will be ‘game changers’ when it comes to fighting back against Britain’s long-running problem of obesity, which costs the economy an estimated £100billion per year.
Hundreds of thousands take the drugs safely and have been doing so for years, which experts say has finally let them shed the pounds that they otherwise could not have shifted.
However, no drug is without risk, health chiefs say.
NHS prescription guidelines are strict, although slimming jabs are available privately for around £200 a month.
People have tricked pharmacists into getting supplies by filling in an online form and lying about their weight and height.
Mr Fry said: ‘It is a huge shame, as in my view Pandora’s Box has been opened up. People can go on the internet and get it there, where people can lie about their weight in order to get it.
‘The drugs must be used by people who are seriously ill with obesity and they should only be used under supervision from a medical professional, but this is not happening.’
He pointed out that the drugs increased in popularity when celebrity A-listers began using them.
Kim Kardashian was one of the first rumoured to have taken it in 2022 when she told Vogue magazine she had lost 16lb in three weeks so she would be thin enough to fit into a dress that once belonged to Marilyn Monroe.
In September 2024, Lottie Moss revealed she was rushed to hospital after suffering an Ozempic overdose when she weighed just 9st.
The model, who is the half sister of Kate Moss, was violently ill, had a seizure and was severely dehydrated after taking the drug.
She was given the jab by a friend who bought it under the counter from a doctor, she claimed.
The NHS currently warns patients to ‘never take an anti-obesity medicine if it has not been prescribed to you’.

Tam Fry, chair of the National Obesity Forum, has warned fat jabs are being used ‘inappropriately’ by non-obese people who ‘fancy losing a bit of weight’
The MHRA notes that the benefits and risks of using these medicines for weight loss by individuals who do not have obesity or a related illness have not been studied.
Experts have called for tighter restrictions on how weight loss drugs are prescribed.
Mr Fry added: ‘The problem is that they work; the genie is out of the bottle, so it is going to be very difficult for the government to stop people using it.
‘In many instances, it is an uncontrolled drug, and we have to get it back under control.’
Meanwhile, there are concerns that illegal knock-off versions of the drugs are being increasingly used – often advertised on social media.
But despite the risks, politicians have warmly received the drugs, with Prime Minister Keir Starmer having previously said the medicines ‘could be very important for our economy and for health’.
He and Health Secretary Wes Streeting have suggested they could play a role in supporting people to rejoin the workforce and limit the number of sick days taken across the country.
A spokesman for the Department for Health said: ‘Weight loss drugs can be game changers in tackling obesity where diet and exercise has been tried first, but they are not a quick fix to lose a few pounds.

Health secretary Wes Streeting has said the injections are not ‘cosmetic’ treatments and should only be used by obese people who have failed to shift weight through diet
‘These are licenced medicines and should only be used under medical supervision by those who are eligible.’
Dr Alison Cave, MHRA Chief Safety Officer said: ‘We continually monitor the safety of medicines during their use, including GLP-1 medicines, and we have robust, safety monitoring and surveillance systems in place for all healthcare products.
‘When a safety issue is confirmed, we act promptly to inform patients and healthcare professionals and take appropriate steps to mitigate any identified risk.
‘On the basis of the current evidence, the benefits of GLP-1 medicines outweigh the potential risks when used for the licensed indications.
‘It is very important to note that a report with a fatal outcome does not necessarily mean that it was caused by the medicine, only that the reporter has a suspicion it may have been.
‘We advise anyone who has questions about suspected side effects from GLP-1s to talk to their doctor and to report via our Yellow Card scheme.’
Novo Nordisk, the owner of Ozempic and Wegovy, said: ‘Patient safety is of the utmost importance to Novo Nordisk.
‘We continuously collect safety data on our marketed GLP-1 medicines and work closely with the authorities to ensure patient safety.
‘GLP-1 receptor agonists (GLP-1 RAs) have been used to treat type 2 diabetes for more than 15 years including Novo Nordisk GLP-1 RA products such as semaglutide and liraglutide that have been on the market for more than 10 years.’
Eli Lilly and Company, the owner of Mounjaro, said in a statement: ‘Patient safety is Lilly’s top priority.
‘We take reports regarding patient safety seriously and actively monitor, evaluate, and report safety information for all our medicines.’