Just a few years ago, retired stockbroker Nic Olsen did almost daily sessions on a rowing machine and took regular three-mile walks, as well as ten-mile bike rides at weekends.
Yet he’s recently had to have both his legs amputated as a result of a common blood vessel disorder that affects around one in five people over 60.
It is one of the leading causes of preventable disability and premature death in the UK.
If caught promptly, the condition – peripheral artery disease (PAD) – can be managed with daily tablets and exercise, but it took 29 GP and hospital appointments over four years before Nic was referred to a vascular specialist who diagnosed him. By then it was too late.
As his wife Fiona recalls: ‘I’ll never forget Nic’s screams because of the terrible pain in his feet.
‘At one hospital visit, as a surgeon examined his right foot he applied slight pressure and Nic screamed the hospital down. The nurse nearly fell off her chair due to the noise he made,’ recalls the 68-year-old exam invigilator from Tugby, Leicestershire.
Nic’s initial symptoms were innocuous enough, but were textbook signs of PAD: pain in his leg (his right leg initially) and calf when walking.
‘It was a burning sensation, and I couldn’t tolerate my foot being in bed at night – it was more comfortable to let it hang down outside the bed,’ says Nic.
Over the next two years, as well as both legs now aching, his toes and feet became constantly painful and the skin would split and ulcerate – again, textbook signs of the condition.
‘Even the pressure of a sheet over my feet would be unbearable,’ says Nic. He was referred to a pain management clinic and multiple healthcare professionals, from podiatrists to physiotherapists and orthopaedic specialists.
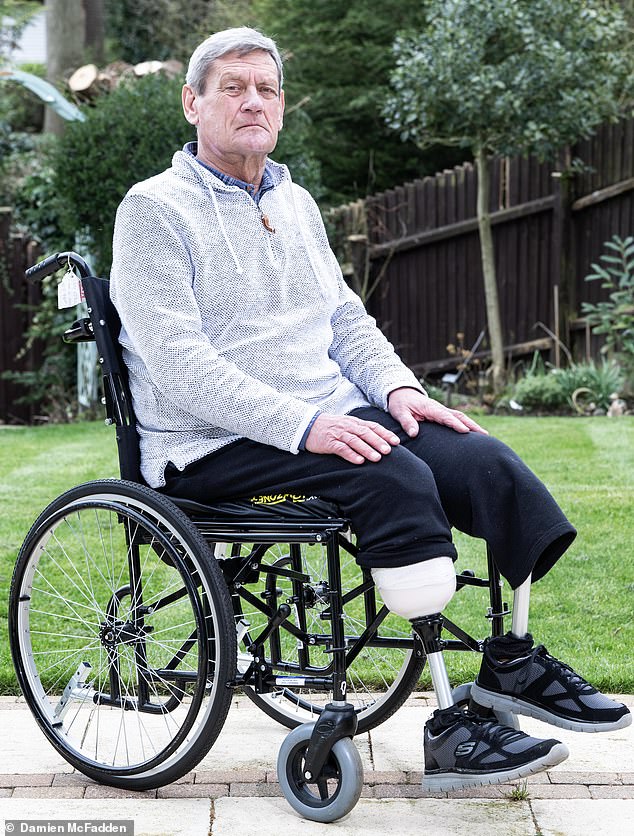
Retired stockbroker Nic Olsen, 80, recently had to have both his legs amputated due to PAD
For three years, doctors thought his pain was due to a problem with his back – and he underwent an MRI, bone density scans and nerve function tests.
He even had spinal surgery in June 2024. The surgeon ‘opened up my spine, hoping to clear debris – that was the exact term he used – but it didn’t help’, says Nic. That’s little surprise, given he didn’t even have a back problem.
PAD occurs when blood vessels supplying the legs become ‘furred’ or narrowed by deposits, just as can happen in the arteries supplying the heart (it can also affect the arms but it’s much less common).
This in turn restricts blood flow to the legs, causing nerve damage and pain, cold toes and non-healing sores.
By the time Nic was correctly diagnosed in November 2024, the three major arteries in his lower legs were almost completely blocked.
Within months he needed his right leg amputated, and then his left leg, too – and the former fitness fan had to face life as a double amputee.
‘I felt my life was over,’ says Nic, now 80, a father of three and a grandfather, eight months on.
‘We were very active, social people before this. We travelled abroad a lot and went caravanning. I can’t see that happening again. I can’t help but think things could have been different if my symptoms were recognised earlier,’ he adds. ‘I feel very let down.’
Nic’s is a horrifyingly common story – thousands of people each year in the UK undergo avoidable leg amputations. There are more than 5,676 leg amputations in England, Wales and Scotland annually. That’s more than 100 a week, with the number growing.
The vast majority of these are due to PAD, says Professor Athanasios Saratzis, an honorary consultant vascular and endovascular surgeon at University Hospitals of Leicester NHS Trust.
‘But if we picked up PAD earlier, we can manage the condition with medication and exercise.’
PAD is essentially like heart disease in the legs. Treatment includes tablets – clopidogrel, a blood-thinner to prevent clots blocking the narrowed arteries, and a statin to reduce cholesterol to minimise further furring – as well as daily exercise to get blood pumping through the legs and keep tissues healthy.
It may be possible to clear mild blockages in the legs, or bypass blocked blood vessels with those from elsewhere, but if these fail it can lead to agonising pain due to tissue death – and the only treatment option then is amputation.
Today, a coalition of experts have written to the health secretary Wes Streeting – in a letter shared exclusively with the Daily Mail – calling for him to implement the recommendations of their report, Making the Case for Reform in the Vascular Sector. This includes improving access to urgent foot care to end the high rate of avoidable lower- limb amputations in the NHS.

NIc’s wife Fiona recalls: ‘I’ll never forget Nic’s screams because of the terrible pain in his feet’

‘We were very active and social people before this who travelled abroad a lot,’ says Nic
This would involve establishing a dedicated Foot Protection Service in every region of the NHS, with rapid access to specialist advice, imaging and treatment – and launching a public awareness campaign on the need to seek help for urgent foot problems.
The letter’s authors include experts from the Royal College of Podiatry as well as Professor Stella Vig, a consultant vascular and general surgeon at Croydon Health Services NHS Trust (she is also the National Clinical Director for Elective Care, NHS England, but is not a signatory in this capacity). ‘Too many people continue to experience delayed diagnosis, fragmented referral pathways and inconsistent access to specialist care,’ the letter warns.
‘The consequences are stark: avoidable harm, prolonged hospital stays and thousands of lower- limb amputations each year.’
The first sign of PAD is usually calf pain on walking, says Rachael Forsythe, a consultant vascular surgeon and chair of the Circulation Foundation, a charity that funds research into preventing vascular disease.
‘At the mild end, you get intermittent claudication – calf pain when you walk and it’s reproducible, meaning it happens at the same distance every time and goes away when you stop. It’s worse when walking up hill.’
Professor Saratzis adds: ‘You get pain in your calves because there’s not enough energy [i.e. oxygen and nutrients]. Your skin and muscles are dying, and they’re trying to tell you “help!”.
Left untreated, symptoms can progress to include ‘pain at rest, a wound that doesn’t heal after four weeks, or foot pain at night – typically they have to hang the leg outside of the bed, using gravity to get the blood down to the foot,’ says Miss Forsythe.
These patients, who account for 5 to 10 per cent of all cases, are at high risk of amputation, she adds, as lack of blood flow can ultimately lead to gangrene.
‘Sometimes, when you open up an artery, it’s like bone – you can tap on this big chunk of hard, rock-like substance in the artery – so you can understand why blood won’t flow through that.’
Known as critical limb-threatening ischaemia, those affected ‘have a worse life expectancy than those with most common cancers’, says Miss Forsythe.
She says the death rates linked to PAD should be a wake-up call for patients and medics.
‘Following a leg amputation, your risk of dying within 30 days is about 8 to 10 per cent; after a year it’s more than 25 per cent – and more than 50 per cent of patients are dead after five years.
Most people don’t know that – even some of my hospital colleagues [in other specialties].’
Miss Forsythe adds: ‘Amputation can be necessary when you’ve exhausted all other avenues. But it’s difficult to look around a ward and know that once someone’s had one amputation, the risk of the other leg coming off in the near future is quite high [because PAD usually affects both legs].’
Risk factors are the same as for heart disease and include smoking, high blood pressure, high cholesterol and diabetes (while smoking rates are decreasing, PAD is increasing due to rising rates of diabetes).
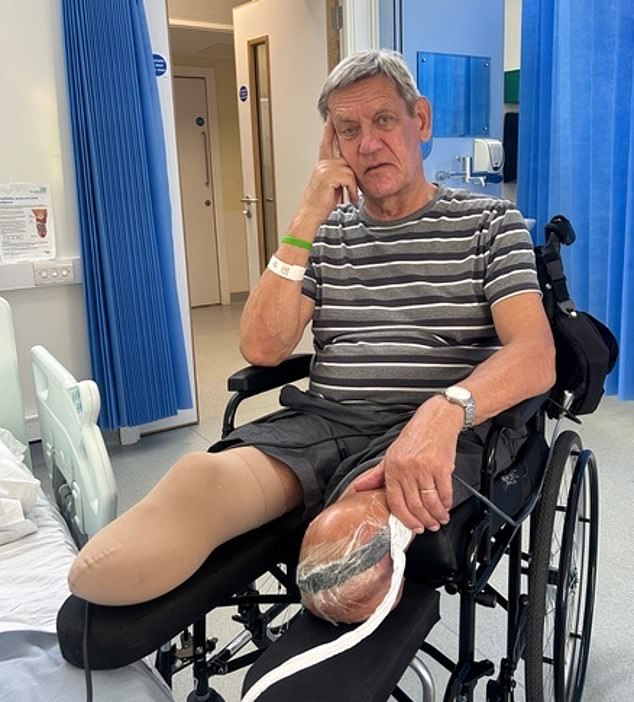
Nic’s is a common story… thousands of Britons undergo avoidable leg amputations each year
‘We’re likely to see increasing numbers, and at younger ages,’ says Miss Forsythe.
High blood sugar damages and narrows the artery walls.
However, the concern is that many diagnosed with heart disease may be unaware of the risk to their legs, suggests Professor Saratzis.
‘People with heart problems are far more likely to develop PAD and we also know that those with PAD are very likely to also have heart issues,’ he says.
‘The reason why we’re likely to know about heart problems earlier is because there’s more straightforward screening – you get tested at age 40 for cholesterol, and if it is very high, then your healthcare provider will probably start thinking about heart issues – but they don’t necessarily think about PAD. That’s where the problem lies.’
And often the condition goes undiagnosed until this late stage, says Professor Saratzis, because ‘you can’t diagnose PAD with a simple blood test or scan’.
He explains: ‘You need to ask the patient the right questions, and examine their legs and their feet. A Doppler test [using a handheld ultrasound to assess blood flow through the arteries] can help, but on its own it’s not enough to make a diagnosis.’
And by the time that diagnosis comes, it can be too late.
When Nic was finally diagnosed (a podiatrist performed a Doppler test and referred him to a vascular surgeon), he was put on clopidogrel and told to walk 10,000 steps per day, to help push blood through the leg arteries.
But the pain was ‘unbearable’ – and three months later, he collapsed in the street.
Nic underwent angioplasty (where a catheter with a small balloon is inserted via an artery in the groin to clear blockages).
‘But my arteries were so badly blocked, they couldn’t get the catheter in – the only option was to try bypass surgery,’ he recalls.
Nic’s blocked arteries would be ‘bypassed’ by using one of his leg veins, replumbing it to carry blood around the blockage.
But three weeks after the surgery, ‘the pain just got worse and worse and the wounds just wouldn’t heal’, recalls Nic.
With no other options, his right leg below the knee was amputated in April 2025.
‘It seemed like the only way out,’ he says. Two weeks after getting home, however, his left leg started to worsen, following the same pattern.
‘The arteries were blocked and my foot was very painful and the skin just split open,’ he says.
Fiona recalls: ‘That was just the worst thing ever. He was screaming in pain. It was unbearable for both of us.’
After an emergency eight-hour bypass operation failed, Nic’s left leg was amputated in July 2025.

Nic says Fiona ‘does all she can, but her life has changed into being a carer’. He hopes sharing his story will alert others to PAD.
Today, he can take only a few steps using prosthetic limbs and a walking frame, and needs a wheelchair even at home. It is a far cry from the happy lifestyle he so recently enjoyed.
‘At my age, prosthetics are very hard,’ he adds. ‘Getting them on and off is difficult and, at times, they hurt. I’m always afraid of falling and therefore use my wheelchair a lot.’
Nic says Fiona – the couple have been married for 37 years – ‘does all she can, but her life has changed into being a carer’.
Losing a limb is ‘a devastating blow to mobility and independence’, says Miss Forsythe.
‘While some are able to regain mobility and get back to a good quality of life, many become dependent on others, and some end up bedbound.’
As well as causing personal misery, the cost to the NHS is high.
‘Each amputation for PAD costs around £18,000, including operating theatre time, staff costs and other costs,’ says Professor Saratzis. ‘On top of that, there are the costs of community visits and wound management before and after surgery.’
The NHS spent £8.3billion on wound care alone in 2017 to 2018.
‘All that money could be saved and redirected to screening and early intervention,’ adds Professor Saratzis.
Currently, if people have foot problems, they’ll typically be reliant on their GP to refer them to a specialist.
But Professor Saratzis says access to specialist care is a postcode lottery.
Under the new proposals, people with chronic foot problems such as hanging their legs out of bed at night to get comfortable (see box) would be able to access a specialist service – and follow a ‘foot attack pathway’ without needing a hospital referral.
You’d be seen the same day or next day within the community, by a podiatrist or specialist nurse – and if you needed urgent vascular assessment with a doctor, you would get that within two weeks (or five days if you’re already a hospital inpatient).
If you needed surgery to unblock blood vessels this would be done within five days of emergency admission, as set out in national guidelines. But figures from the National Vascular Registry show only half of patients are treated within this timeframe.
Professor Vig called the report a ‘once-in-a-decade opportunity to improve vascular care for patients right across the country. In order to save their limbs and lives, we have to act now,’ she told Good Health.
Nic hopes sharing his story will alert others to PAD.
He’s now focused on getting mobile enough to walk his daughter down the aisle at her wedding in Greece this summer, with physio and weekly gym visits.
‘It makes me very sad to think that early diagnosis might have saved my legs,’ says Nic. ‘PAD can affect even fit people like me, so doctors need to look beyond typical risk factors.’
Fiona adds: ‘I think one mistake we made was constantly seeing the same GP. We trusted in all the healthcare professionals we saw but, on reflection, I don’t think the system as a whole worked well for us. ’












