A BRAIN “pacemaker” has helped over a third of severely depressed patients all but wipe out their symptoms.
Scientists say 34.6 pe cent of people in the trial went into remission, meaning a near-complete elimination of their symptoms, after receiving deep-brain stimulation (DBS).
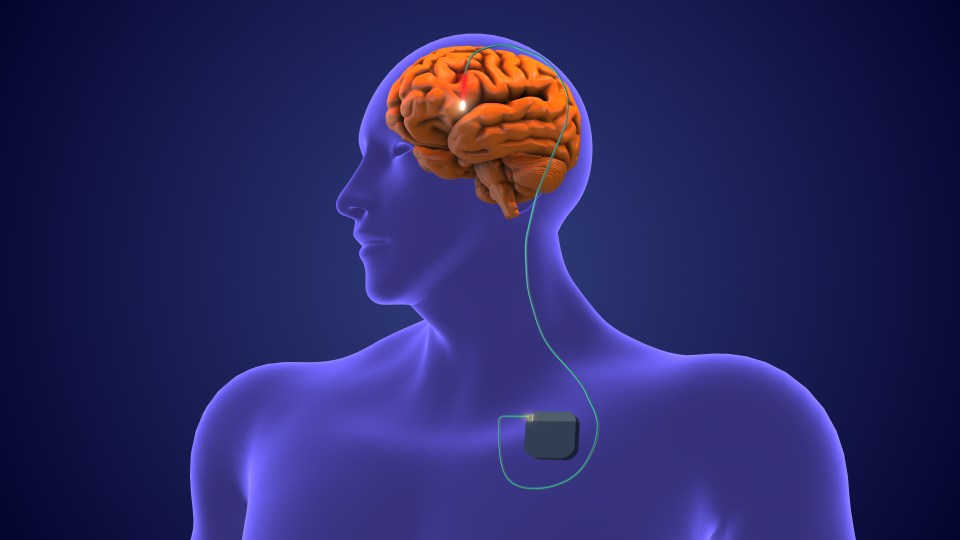
The device works like a brain-based “pacemaker”, sending controlled electrical signals that helped one in two people with treatment-resistant severe depression in the trial.
The study, led by researchers in the UK and China, also identified a “tell-tale” signature of brain activity that predicted how well individual patients responded to the treatment.
The breakthrough could be used in future to allow personalised treatment of those patients most likely to benefit, say scientists.
Major depressive disorder is one of the most common mental health problems worldwide.
While antidepressants and cognitive therapies help many sufferers, there are still high rates of treatment resistance with current methods failing for between three and five patients with depression.
DBS has begun to be used in recent years to treat a range of conditions, most successfully for patients with Parkinson’s disease.
The technique involves the insertion of thin electrodes deep into the brain that transmit mild electrical stimulation to correct errant brain activity.
For the new study, researchers trialled DBS in 26 patients recruited from Ruijin Hospital, Shanghai Jiaotong University School of Medicine in China, all of whom had treatment-resistant depression.
The trial was “open label”, which means both researchers and the patients were aware that DBS was being administered.
The team applied stimulation to two areas of the brain.
The first was the bed nucleus of the stria terminalis (BNST), an extension of the amygdala that is involved in regulating stress, anxiety, fear and social behaviours, particularly in response to long-term stresses and fears.
The second area was the nucleus accumbens, which is involved in how the brain processes rewards, and is a key area for motivation, pleasure, and reinforcement.
Half of the patients (13 out of 26) saw “significant” improvements, as measured on different scores for depression and anxiety-related symptoms along with clinically relevant quality of life and disability scores.
Nine of those patients achieved remission, according to the findings published in the journal Nature Communications.
‘Real promise’
The research team recorded brain electrical activity from the DBS electrodes in the BNST and scalp EEG (electroencephalogram) and found brain activity at a specific frequency range (4-8 Hz), known as theta activity, to be clinically important.
Theta activity in the BNST correlated with how severe a patient’s depression was and how anxious they felt on a daily basis – those patients with higher levels of theta activity experienced worse symptoms.
People with lower levels of theta activity in that brain region before surgery tended to improve more and report greater improvements in quality of life at three, six and 12 months, though only in relation to depression and anxiety, not to loss of pleasure.
Those patients with greater “coherence” between the BNST and the prefrontal cortex in theta frequences – in other words, those where these two regions were most closely synchronised – were also likely to have better outcomes.
The prefrontal cortex is involved in emotional regulation, and greater coherence implies better communication between these two regions.
Professor Valerie Voon, of Cambridge University and Fudan University, China, said: “Deep brain stimulation shows real promise at tackling treatment-resistant depression, which can have a huge impact on people’s lives.
“But our study hasn’t just highlighted this promise, it’s given us a potential and much-needed objective marker to say which patients will respond best.”
Signs and symptoms of depression
You may feel:
- Continuously low or sad
- Hopeless
- Tearful
- Anxious
You may have:
- No motivation or interest in things, such as hobbies
- Suicidal thoughts
- Lack of appetite and energy
- Disturbed sleep
- Urge to avoid friends or socialising
If you or someone you know is experiencing a mental health problem, the following organisations have more information or can help:
Mind: mind.org.uk, 0300 123 3393
Rethink Mental Illness: rethink.org, 0300 5000 927
Samaritans: samaritans.org, 116 123
Dr Linbin Wang, from the department of psychiatry at the University of Cambridge said: “We found that brain activity at a particular frequency – theta brainwaves – could tell us which patients would have the best response to DBS treatment in the BNST brain region.
“This could help us personalise treatment for individual patients in future.”
During the trial, DBS reduced BNST theta activity, and that reduction matched improvements in symptoms of depression and anxiety.
That opens up the possibility of using a ‘closed-loop system’ that uses real-time feedback to adjust the electrical stimulation, according to the research team.
Prof Voon said: “Because theta activity tracks anxiety states in real time, it means that if activity is high, we can say ‘OK, this person is an anxious state, we need to turn up stimulation’.
“Likewise, if theta activity is low, we can turn down the stimulation.”
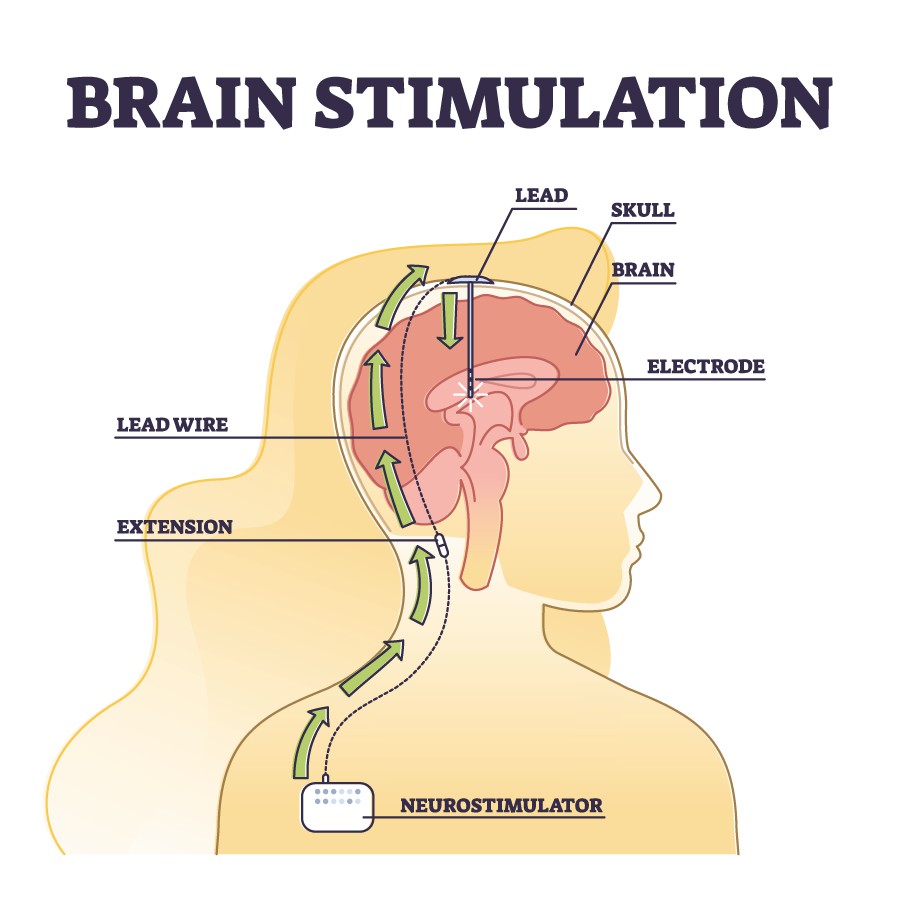
What is deep-brain stimuation and what is it used for?
DEEP brain stimulation (DBS) involves implanting electrodes within areas of the brain
The electrodes produce electrical impulses that affect brain activity to treat certain medical conditions.
The electrical impulses can also affect cells and chemicals within the brain that cause medical conditions.
The amount of stimulation in deep brain stimulation is controlled by a pacemaker-like device placed under the skin in the upper chest.
A wire that travels under the skin connects this device to the electrodes in the brain.
Deep brain stimulation is commonly used to treat a number of conditions, such as:
- Parkinson’s disease.
- Essential tremor
- Conditions that cause dystonia, such as Meige syndrome
- Epilepsy
- Tourette syndrome.
- Obsessive-compulsive disorder
Deep brain stimulation also is being studied as a potential treatment for:
- Chorea, such as Huntington’s disease
- Chronic pain
- Cluster headache
- Dementia
- Depression
- Addiction
- Obesity
Source: Mayo Clinic
Professor Bomin Sun, the neurosurgeon who led the research at Shanghai Jiao Tong University School of Medicine, said: “This is the largest study to show that deep brain stimulation of the BNST and nucleus accumbens can treat depression.
“Depression is a major public health problem in China and globally.”
He added: “This study not only tells us how the brain is impaired in depression, it also highlights potential of DBS for depression.”
The team also found psychological measures that indicated how well a patient would respond to treatment.
Participants were shown a series of images, some pleasant – such as puppies, some neutral – such as furniture, and some negative – such as accidents.
Patients with the strongest reaction to the negative images were least likely to see benefits from DBS, according to the findings.
















