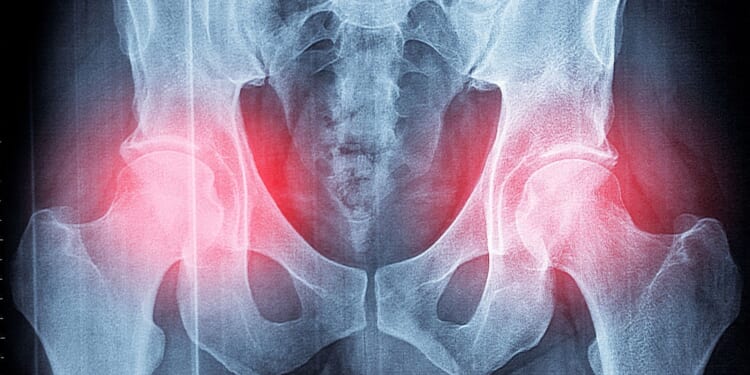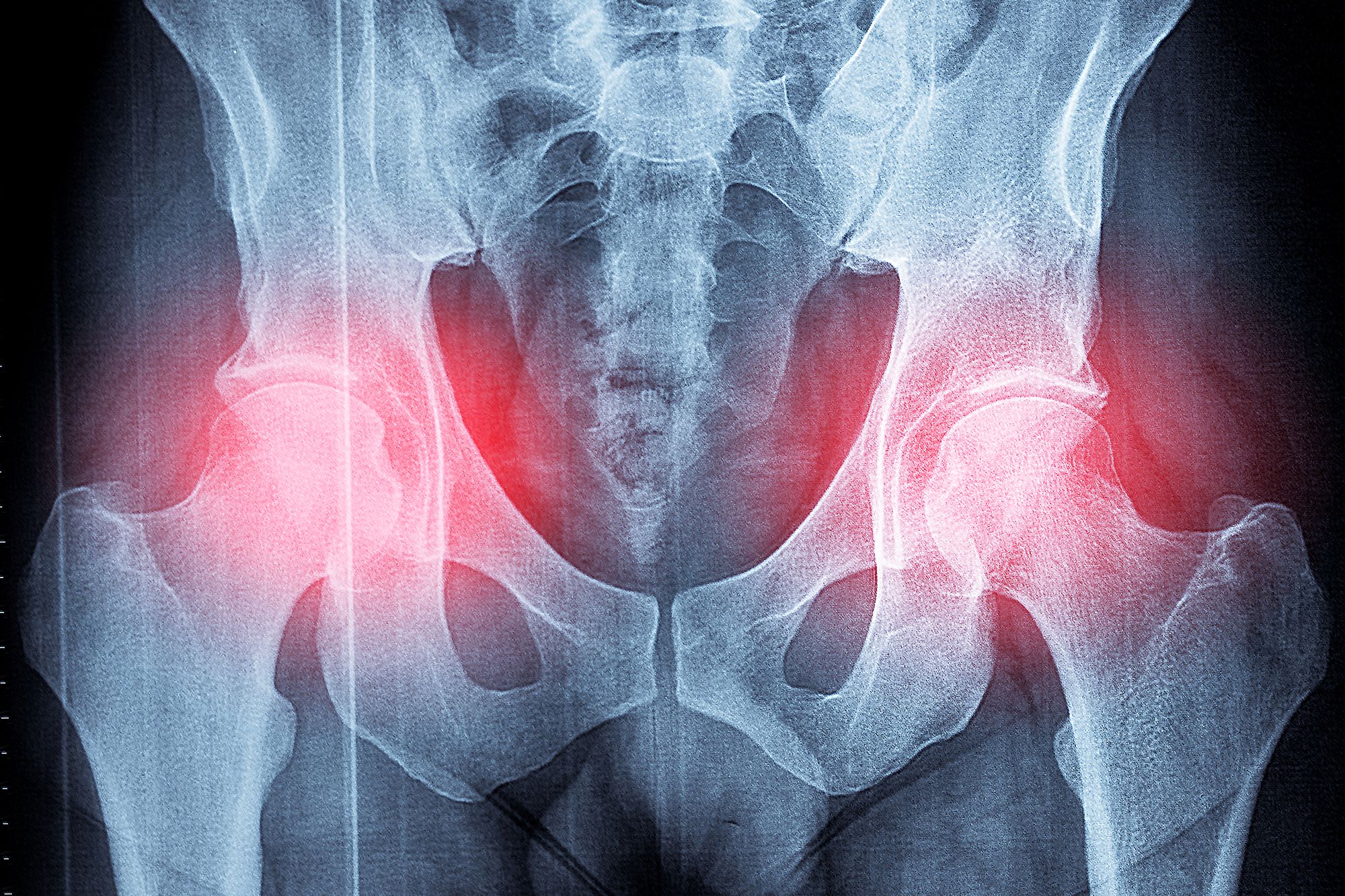
NEARLY one in five NHS organisations denying patients knee and hip replacement surgery because of their weight, a new report shows.
The practice is leaving people needing the operations at risk of more pain, Arthritis UK has warned.
The charity also raised concerns that these policies are being implemented “in a bid to cut waiting lists and costs”.
Thirty-one of 42 NHS integrated care boards (ICBs) – NHS organisations responsible for planning health services for their local population – have joint replacement op policies relating to to body mass index (BMI), analysis by Arthritis UK found.
According to the charity, eight ICBs (19 per cent) won’t refer patients above certain BMI thresholds for surgery – meaning they are “rationing” procedures based on weight.
A further 23 have policies that encourage or require patients to lose weight to become eligible for these operations, the report said.
Only 11 ICBs don’t restrict or alter access to joint replacement surgery based on BMI.
ICBs justify the use of BMI policies by pointing out potential risks to patients, the charity said.
But it said surgery is only risky to people with a very high BMI, according to research.
Arthritis UK said policies have “been inappropriately used” to cut off patients with lower BMIs, affecting thousands “who would have received the significant improvements in their joint pain and function”.
The National Institue for Health and Care Excellence (Nice) advises against using BMI to exclude patients from referral to surgery.
Deborah Alsina, chief executive of Arthritis UK, said: “This practice is unfair and flies in the face of all guidelines and evidence.
“People waiting for joint replacement surgery, often due to arthritis, have already spent many months or years with their health and mobility in decline as joint replacement surgery is the final line of treatment.
“Joints in need of replacement are incredibly painful and severely impact the ability of individuals to exercise which can lead to weight gain.
“It is counterproductive to deny surgery that could get people back on the road to mobility and improved health and fitness.”
Arthritis UK claims that BMI policies “are often ambiguous in their requirements” and can be open to interpretation by clinicians “leaving patients without a clear understanding of what is expected of them”.
Among the ICBs applying BMI thresholds, there is a “significant variation on the cut-off point”, the report added.
Arthritis UK is calling for an end to BMI policies that restrict access to surgery.
The new report has also been backed by The Royal College of Surgeons of England and the British Orthopaedic Association.
Fergal Monsell, surgeon and president of the British Orthopaedic Association, said: “Improving someone’s health before planned surgery is usually helpful.
“However, losing weight is not always easy and may not significantly lower the risks of surgery.
“Refusing or delaying surgery until a patient loses weight could be seen as unfair.
“In fact, waiting to have surgery while trying to lose weight may make patients less fit, increase their pain and disability, and reduce their overall physical condition.
“Denying someone the benefits of planned orthopaedic surgery based only on BMI is not evidence-based, and differences in rules across the UK mean access to treatment can depend on where someone lives, resulting in a ‘postcode lottery’.”
Tim Mitchell, president of the Royal College of Surgeons of England, added: “Supporting patients to reach a healthier weight before surgery can reduce complications, but BMI alone should not be a barrier to surgery.
“Surgical decisions must be made case by case, reflecting each patient’s individual circumstances.”
Mr Mitchell said that timely surgery “can significantly improve a patient’s quality of life” while delays can lead to loss of mobility and further health problems.
“We must not penalise those who are less fit but still eligible for an operation,” he added.
“ICB policies that do this are unfair and ignore clinical guidance.”
Arthritis UK also raised concerns that ICBs are using BMI policies to cut costs and waiting lists, and called on the Department for Health and Social Care to ensure that cutting waits are not “to the detriment of a patient’s wellbeing”.