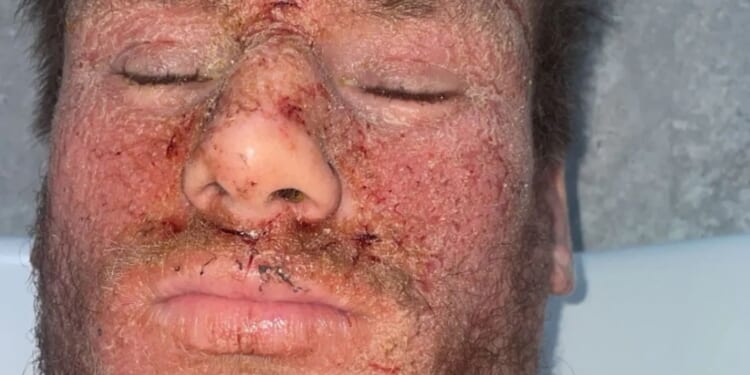
A YOUNG dad who used a commonly prescribed cream for a year has told how he was left “screaming in agony” and bedbound for six months after suffering a horrific reaction when he stopped using it.
Callum Hobson, from Hull, was first prescribed the steroid cream in December 2022 to help treat blemishes on his arms caused by fibreglass insulation when working as an electrician.
The now 25-year-old was then re-prescribed it throughout the year, not realising it isn’t recommended for use beyond five days and claimed he wasn’t warned by doctors of the risks of overuse.
It was only after he began experiencing rashes that re-emerged stronger and more painful every time he stopped using the cream, that he came off it completely in November 2023, fearing he was suffering topical steroid withdrawal.
The condition, thought to affect hundreds of thousands of people every year, occurs when patients reduce or stop steroids.
Skin can react violently, becoming red, burning, painfully dry and intensely itchy, trapping patients in a cycle whereby starting steroid creams is the only relief from symptoms.
Now, Callum has told how he feels he has “lost” the past three years of his life trying to treat the symptoms of topical steroid withdrawal.
His condition meant he even missed the birth of his 11-month-old daughter, Maddy, in April 2025 after being left bed bound for six months.
To date, Callum has spent £10,000 on treatment and is currently crowdfunding for a further £5,000 so he can “get over the finish line”.
Recalling his horrifying ordeal, he said: “I was so ill and my skin was so bad I couldn’t open my mouth without severe pain.
“At my worst I was only eating every couple of days, and because of it I dropped six stone in weight from 11 stone to seven stone.
“My life fell to bits, I couldn’t get out of bed never mind walk.
“It was so preventable which is the thing that hurts the most. I wouldn’t wish it on my worst enemy.
“But I want to raise awareness to prevent people from falling into the same situation I did.”
He had never had issues with his skin growing up, he said, including not suffering acne as a teenager.
But, in mid 2022 aged just 22, he began developing itchy eczema-like rashes on the inside of his arms leading to him to go to the doctors to get it treated.
Here, doctors proscribed him steroid cream to deal with the rashes.
Callum’s recalled the GP telling him to use it “as and when” he needed to calm down the itching and pain they caused.
He used the cream “every other week” to deal with rashes which formed on his arms, and then his face, even though he didn’t realise wasn’t supposed to.
He claimed that whenever he ran out of cream or if the rashes re-emerged, he called the doctors and they either re-prescribed or prescribed a cream with a higher dosage.
Callum said: “The cream would work for a week causing the blemish to go away and before I knew it a week later it was back.
“The doctors were just happy to prescribed me more and more, this went on for a year.
“At the time, I had no idea of the consequences of long-term use, but the doctors must have, yet they never pulled me in for a review or consultation to change the treatment.”
In November 2023, Callum’s girlfriend Olivia Tweddell, 25, was studying biomedical science at Hull University and the side affects of long-term use of steroid cream was raised in one of her classes.
Callum then came off the cream completely and a month later his skin went into a “melt down”, he said.
His face, chest, arms, and legs developed itchy painful, oozing sores.
In February 2024, his girlfriend rushed him to hospital thinking he was suffering from sepsis after his leg turned a “strange purple colour”.
He then spent a week at Hull Royal Infirmary where he was given oral steroids, antibiotics, and immunosuppressants to treat his skin.
Despite this, his skin suddenly flared up shortly after being discharged and after it continued to deteriorate he left his job as an electrician and became bedbound.
Callum said: “Missing my daughter’s birth was tough.
“I had to keep coming and going from the hospital to wipe cream off of my skin, wash it, get dressed and head back.
“On one of those occasions Maddy was born, I have missed events due to my skins but this was by far the biggest.
“Then not being able to hold her because of how painful it would have been, it was just heartbreaking.
“Liv had to do everything – wash me, feed me, as well as balancing her job and looking after our daughter.
“She really is a superstar, sacrificing everything for me, I might not be alive without her.
“I would wake up in a swell of blood and cream, taking off the covers felt like it was ripping my skin off.
“It was a horrific time in my life.”
Callum has since set up an Instagram page – cal_tsw – to raise awareness for the issue.
He has also started cold atmospheric plasma (CAP) therapy to treat his skin.
CAP is a non invasive treatment which works by reducing inflammation, killing bacteria, heals wounds, and improving the skin barrier, according to the NHS.
Callum undergoes the treatment – which lasts 35 to 45 minutes – privately, which cost £500 a session.
He has already had 20 session spending £10,000.
Callum added that he believes he is now 80 per cent healed and needsfurther therapy on hands and face, which are “struggling” the most.
He is currently crowdfunding to raise a further £5000 in the hope of having 10 more sessions which should “push him over the finish line”.
He said: “I think I’m almost there now, I feel like I have nearly got my life back.
“It is just my hands and face now.
“I think if I had 10 more sessions, it will get me there, then I will just be tasked with maintaining my skins health.”
Topical steroid withdrawal was recognised by the National Eczema Association in 2013.
Also known as red skin syndrome, the disorder does not have clear statistics to show just how common it is.
But one 2003 study from Japan, found that 12 per cent of adults who were taking steroids to treat dermatitis developed red skin syndrome.
In 2018, the medical journal Dermatitis published the results of a three-year study of Australian patients presenting with TSW and acknowledged that it is often dismissed as being a result of over-use of steroids, or even steroid phobia.
The British Association of Dermatologists accept that doctors still do not recognise this condition.
Steroids — including creams, lotions or gels — often do not cause side effects if they are taken for a short time, but if a high dose is taken for a longer time, there is a higher chance of getting more serious side effects.
Most people will not have side effects when they stop taking steroid medication, the NHS says, but it is important to follow advice from doctors as patients may need to reduce their dose gradually.