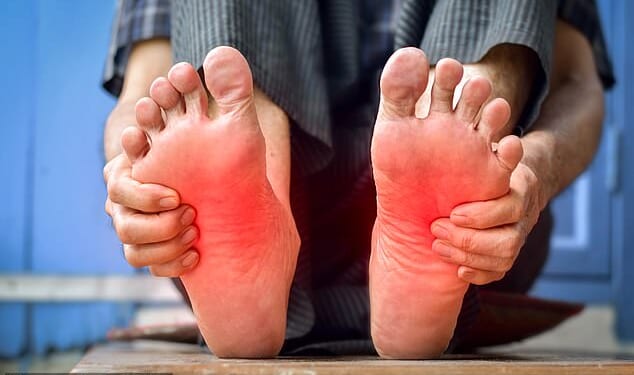
I have started experiencing a burning sensation in my feet. I take no medication, and while I am 86 I’m otherwise healthy. What could be the cause?
Dr Philippa Kaye answers: A burning sensation in the feet is likely to be caused by a nerve condition called peripheral neuropathy.
Nerves are responsible for controlling all movements and sensations, including pain, temperature and touch.
But if they become damaged or are under pressure, they don’t function properly.
The most common cause of peripheral neuropathy, which also affects hands, is the blood sugar condition diabetes. If not treated properly – by getting blood sugar levels down through lifestyle changes and medicine – diabetes can lead to organ and nerve damage, and, in extreme cases, may even lead to the amputation of affected limbs.
A GP can carry out tests to look for signs of diabetes.
Patients should check their feet every day for blisters, cracks, redness or sores, as this might suggest worsening damage caused by diabetes.
Issues in the thyroid – the butterfly-shaped organ in the neck that produces crucial hormones – can also lead to peripheral neuropathy. Hypothyroidism, low thyroid levels, is typically easily treated with medication once spotted. Again, a GP should be able to diagnose this issue.
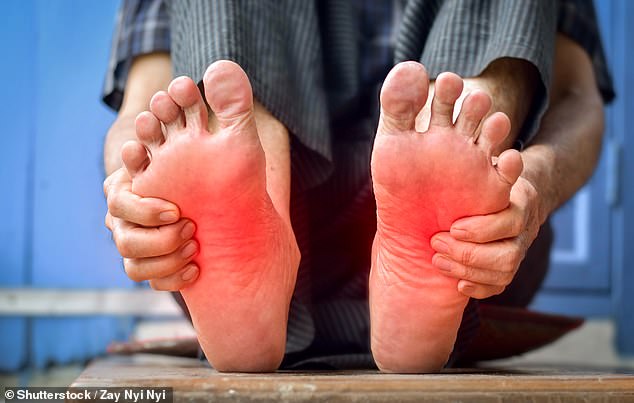
A burning sensation in the feet is likely to be caused by a nerve condition called peripheral neuropathy
Excessive alcohol consumption can also lead to nerve damage.
Another test that a GP can run is to check for a vitamin B12 deficiency. This is a nutrient gained from animal products, such as meat and eggs, that is important for nerve health.
A deficiency can be treated using supplements, which should help with the burning sensation.
While waiting for a diagnosis, there are steps that can be taken to minimise peripheral neuropathy symptoms.
These include wearing comfortable, well-fitting shoes with good cushioning and support. Avoid wearing high heels, as the pressure points can worsen pain, while tight or seamed socks can also further irritate the feet.
Peripheral neuropathy can lead to reduced sensation in the feet, so it’s important to avoid using hot water bottles, heating pads or sitting too close to fires, as serious burns can occur without the body noticing the pain.
Finally, there are drugs that can help combat the pain of peripheral neuropathy.
These include the nerve pain drugs amitriptyline, nortriptyline, and gabapentin.
My daughter, 35, suffers from terrible migraines. I’m desperate for her to have a normal life. What could help?
Dr Philippa Kaye answers: The horrible headache condition can be debilitating but there are effective treatments available on the NHS.
We have medications to help with pain and nausea once a migraine develops. These include triptans – prescription tablets that can stop an attack from developing if taken early enough. Some patients also benefit from taking anti-inflammatory painkillers, like ibuprofen, alongside them, as well as anti-sickness medicines if nausea is an issue.
There are also medications that can reduce the risk of migraines developing, including tablets called beta-blockers and certain anti-seizure medicines.
Interestingly, regular injections of Botox, the cosmetic anti-wrinkle treatment, can also reduce the frequency and severity of migraines. This would need to be administered by a specialist and can, under certain conditions, be offered on the NHS.
There are also injections or infusions called anti-calcitonin gene-related peptides, or anti-CGRP, that can markedly reduce migraines for some patients. Unfortunately they are not effective for everyone, and there is also a very long waiting list to get them on the NHS.
However, there are steps that patients can take themselves to reduce migraines. One of these is identifying triggers – whether that’s too little or too much sleep, stress or certain foods. Likewise, keeping to a routine – waking up, eating and going to bed at roughly the same time each day – has been shown to lessen migraines.
Many patients keep a migraine diary, which involves logging every time a migraine occurs, in order to work out what behaviour or habits are bringing them on.
For more information, visit The Migraine Trust’s website (migrainetrust.org).